
Tuberculosis (TB) affects 10 million people and kills nearly 1.7 million every year making it the leading cause of mortality worldwide from an infectious disease. In Tanzania and elsewhere, the prevalence of TB varies considerably across regions with the presence of other diseases (comorbidities) accounting for different TB treatment outcomes.
Now, scientists from Ifakara Health Institute and Swiss Tropical and Public Health Institute have identified differences in the epidemiology of tuberculosis and comorbidities between rural and urban Tanzania, urging authorities to consider such differences when designing key public health interventions.
Patients from the rural setting had … an overall 6% increase in the odds of recurrent TB for every one year increase in the life of a TB patient from the two settings.
In a publication published in Infectious Disease of Poverty, it was seen that patients from rural Tanzania were likely to be older and at a more advanced stage of illness (i.e., lower body mass index and lower CD4 cell counts for patients with HIV co-infections) as compared to those from urban Tanzania.
Patients from the rural setting had approximately 4 times higher odds of recurrent TB than their counterparts from the urban setting with an overall 6% increase in the odds of recurrent TB for every one year increase in the life of a TB patient from the two settings.
The proportion of HIV infection and diabetes mellitus were similar in the two settings. On the contrary, the urban setting had higher prevalence of helminth infection primarily driven by a particular type of worm infestation known as Strongyloides stercoralis, whereas in the rural setting the main culprit was Schistosoma mansoni which was to be expected due to close proximity of the study area with the Kilombero river.
The higher proportion of helminth co-infection in the urban setting is partly due to an increased proportion of patients who carried an “occupational risk” in the urban setting defined as working in rice fields, car washing, sand harvesting or fishing. Also the urban study site comprises a city experiencing uncontrolled population growth with poor urban planning and hygiene control, all of which propagate helminths infections. These factors could explain the higher proportion of helminths co-infections in the urban Tanzania as opposed to rural Tanzania.
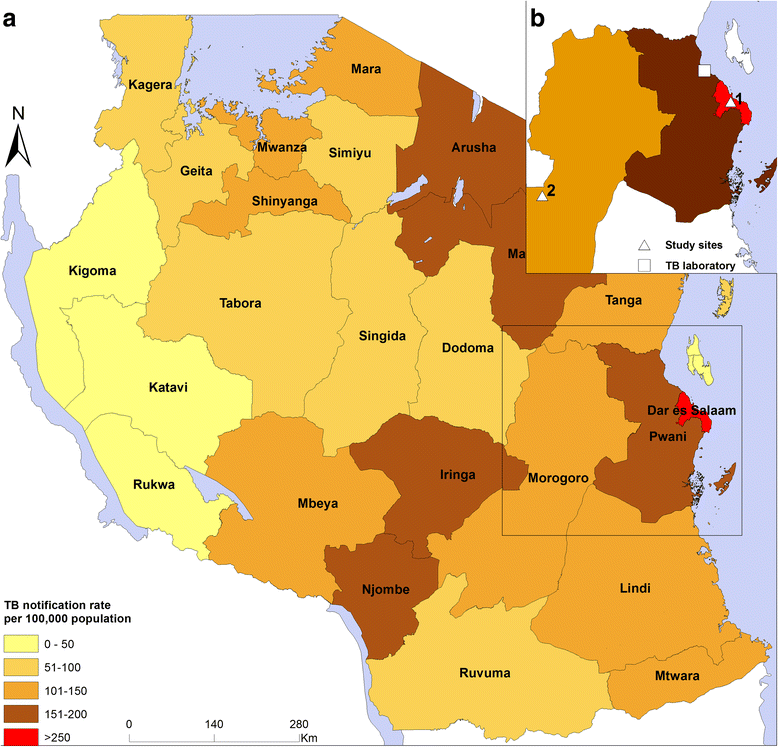
Differences in urban and rural treatment
TB patients from these two settings exhibited different health seeking behavior which could be exploited in efforts to fight TB and co-infections. Nearly a quarter of patients from the rural setting sought care from traditional healers prior to TB diagnosis. This could result in continued TB transmission in the community due to delays in TB diagnosis and presentation at health facilities as an advanced stage of the illness.
Nearly a quarter of patients from the rural setting sought care from traditional healers prior to TB diagnosis.
Patients from the rural setting had individually less access to anti-helminth medication 12 months prior to TB diagnosis. Unfortunately, patients from the rural setting also had less access to mass drug campaigns for helminthiases in the past 12 months prior to TB diagnosis. It is known that comorbidities such as helminthiasis, HIV, diabetes etc., affects treatment outcome, it is vital for the TB control program to take note of such differences that exist between rural and urban setting.
We think that the findings of this study are not specific to Tanzania, but could be true to other settings in sub Saharan Africa and elsewhere hit by the TB epidemic. The observation may guide public health policies which can target, for example, traditional healers aiming to identify TB cases at early stages of the disease or helminth screening and treatment depending on which species predominates a particular setting.
As it has been seen in other studies, only about 20% of TB is transmitted within ones household – a feature predominant in the urban setting. We saw that patients in the rural setting were likely to have contact with a TB patient – making active case finding activities more beneficial and cost effective in the rural setting.
These differences in TB epidemiology and co-infections in urban and rural Tanzania underline the importance of public health interventions that are tailored to a given setting not only in Tanzania but elsewhere in the world.
Comments