
The raging COVID-19 pandemic in North America and Europe in March and April 2020 caused people to shelter-in-place, protecting them from mosquito bites. Later, as lockdowns were gradually lifted, and people started getting outside, mosquitoes had plenty of chance to bite people. However, as the entire public health infrastructure was diverted to respond to the COVID-19 response, there was a concern that lack of attention could lead to potential outbreaks of other diseases. In particular, mosquito- and tick-borne diseases generally receive less attention than directly transmitted pathogens, given that most of these pathogens are not as common. This is a valid concern, already demonstrated in other parts of the world such as a resurgence of dengue and malaria with reduced control and investments.
In North America and Europe, the most important endemic mosquito-borne disease is West Nile virus. West Nile virus was first detected outside of Africa in Europe in the 1960s, and spread more widely in the 1990s and 2000s. It was also introduced into North America through New York in 1999, and quickly spread across the continent, reaching the Pacific coast by 2003. West Nile virus became endemic on both continents, perpetuated locally in a bird-mosquito amplification cycle, spilling over and infecting dead-end hosts such as horses, people, and other mammals. Between 1999 and 2014, 37,000 cases were reported in the United States, 1600 of those involving neurological symptoms, such as meningitis, encephalitis or flaccid paralysis, and causing an estimated economic burden of $778 million in healthcare costs and lost productivity.
There has been large variability in the annual number of reported cases between years both in North America and Europe, partly explained by variation in climate-driven temperature anomalies, viral genetics, as well as ecological factors such as avian host immunity. While there was a hope that case numbers will gradually decline past 2003 in the United States, there was a large outbreak in 2012, when 5,674 cases were reported, 2,873 of which were neuroinvasive, and 286 of those patients died. Similarly, 2018 in Europe proved to be a record year for West Nile virus infections, with 2083 cases and 181 deaths reported, across a large geographic extent of Europe, mainly attributed to ideal climatic conditions such as high temperatures.
Given this large variability in West Nile virus infection rates, and the fact that it has been 8 years since the largest outbreak in North America, it was worrisome this summer that we would get another large West Nile virus outbreak. That would have very difficult, as public health resources have been diverted away from environmental health to COVID-19 response, creating a situation where, potentially, human cases would become the sentinels for WNV transmission between mosquitoes, not the other way around. This was such a concern that a group of mosquito experts at the CDC published a call in the Morbidity and Mortality Weekly Report for the continuation of mosquito and WNV surveillance amid the pandemic. For example, in Spokane County, where I live, staff members at the Spokane Regional Health District who normally deal with Environmental Health have been tasked with COVID-19 response. In addition, the Washington Department of Health has stopped receiving mosquitoes from surveillance partners, such as myself, to identify and test those mosquitoes for West Nile virus. I actually collected mosquitoes using CDC-light and gravid traps in Spokane County, and am still in the process of learning the molecular methods to test them myself for WNV in my lab. That basically left Spokane County without functional West Nile virus surveillance of mosquitoes this summer, so I wouldn’t have noticed a large increase in risk to people. Fortunately, the Mosquito Control Districts in our state still kept collecting and testing mosquitoes, and providing data to the State and the CDC.
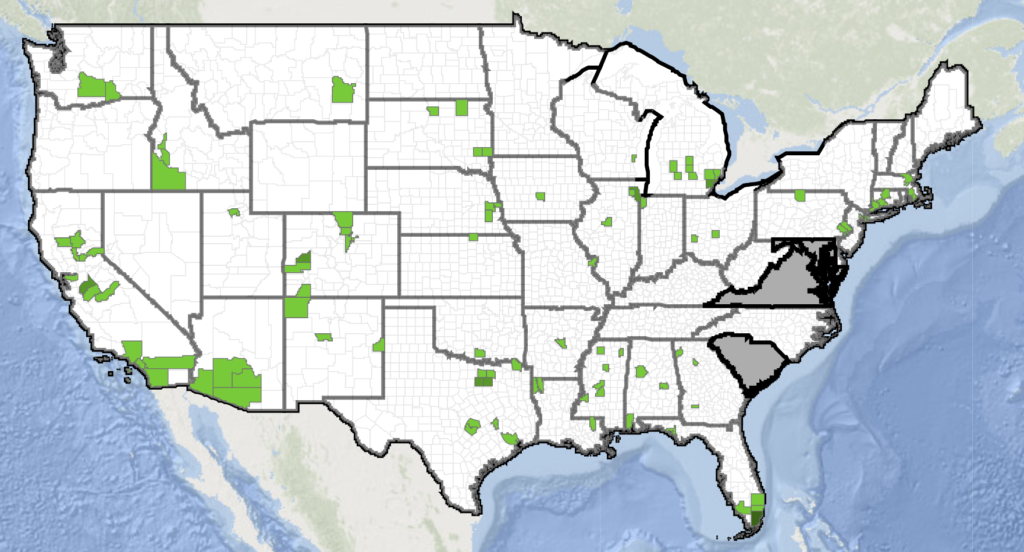
At this point, it seems like that we got lucky, and there hasn’t been a large outbreak of WNV, neither in North America, nor in Europe. As of October 6, 2020, only 279 cases of West Nile virus disease have been reported in the United States, of which 212 were neuroinvasive; however, cases were spread across the US. There were generally low numbers of WNV detections in horses and mosquitoes as well, although the latter could have been a side effect of limited surveillance.
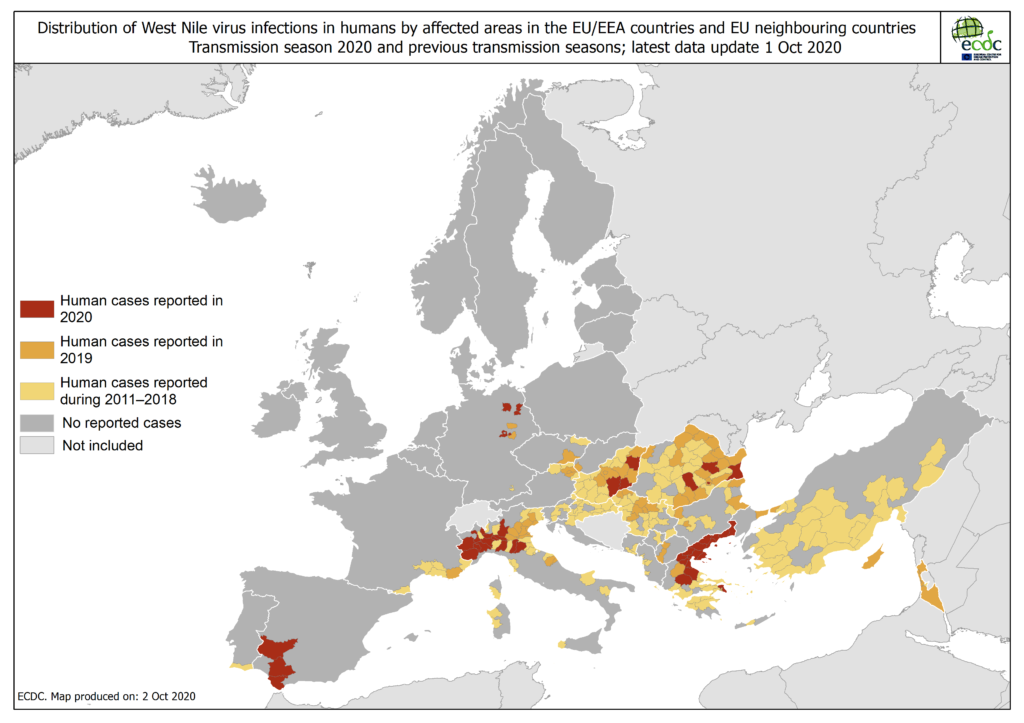
In Europe, as of October 1, 2020, EU Member States reported 257 cases and 30 deaths, most of them in Greece, Italy and Spain, almost 10 times less cases and deaths than in 2018. In addition, the geographic area where WNV cases were reported were also much smaller than in 2018, except for a few areas in Germany and Spain, from where WNV cases have not yet been reported before.
Why did we get so lucky? I’m not quite sure. However, one of the factors cited as causing the massive WNV outbreak in the United States was a prolonged drought. This might seem counterintuitive, as mosquito larvae need water to develop in. However, the main vectors of West Nile virus, Culex mosquitoes, need high nutrient levels in their breeding sites, which get concentrated in conditions of drought. In addition, drought conditions concentrate birds and mosquitoes around the last few remaining wet areas, supercharging the amplification cycle. These features lead to both increased Culex abundance and West Nile virus levels during drought conditions. Comparing the drought maps of 2012 and 2020 for the United States, one can see that there was a much more severe and widespread drought in 2012 compared to 2020. So we might have been saved by less heat and more rain!
Of course, the mosquito and West Nile virus season in North America and Europe is not quite over, and there might be additional human cases still reported in the next few weeks. However, it’s unlikely that this overall trend will change.
We should take our luck with mosquitoes and West Nile virus this summer in our stride, and make sure we build back our mosquito and West Nile virus surveillance capacity that we lost this summer. I will certainly work hard on getting my lab ready to test the mosquitoes I collect in Spokane County next year, and I also hope that the Washington Department of Health will reestablish their capacity to identify and test mosquitoes for West Nile. Ultimately, I do hope that the COVID-19 pandemic will lead our society to appreciate more the importance of disease surveillance and be willing to invest more money in maintaining it.

Comments