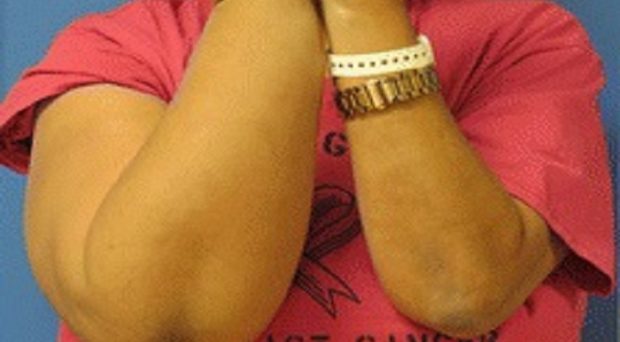
Lymphedema represents a generalized buildup of extracellular lymph fluid within the soft tissues of arms and legs. This results from an imbalance in the amount of lymphatic fluid that is being produced and the amount of lymphatic fluid that is being cleared from lymphatic channels into the venous circulatory system.
Lymphedema is categorized as either primary lymphedema or secondary lymphedema. Primary lymphedema is a relatively rare condition and results from intrinsic structural or functional issues in the lymphatic drainage system secondary to abnormalities in the structure and/or function of the lymphatic channels.
Secondary lymphedema is far more common and is the result of extrinsic disruption in lymphatic transport. In the more developed western world, this is most frequently caused by the traumatic surgical disruption of the normal lymphatic pathways. Cancer treatment, especially surgery and radiation therapy can result in the development of lymphedema. Breast cancer surgery is the most common cause of secondary lymphedema in the arms. atients whose axillary lymph nodes are removed or irradiated as part of their therapy are at particularly high risk of developing this condition, which can arise years after surgery. Lymphedema in the legs is most commonly associated with gynecologic cancers, urologic cancers, melanoma, and lymphoma.
Lymphedema has a major impact on the quality of life of affected patients, both in terms of increased morbidity and significant psychological effects. The skin and soft tissues of the affected limb become progressively swollen, firm, and tight feeling due to the buildup of entrapped lymphatic fluids. The swelling can feel uncomfortable or even painful, and may make movements more difficult. Most seriously, this condition makes the affected limb much more prone to repeated and potentially life-threatening skin and soft tissue infections. Many patients eventually develop depression as a consequence of the impact that lymphedema has on their well-being and their physical appearance.
Currently, there is no cure for lymphedema, which will affect patients for the rest of their lives. However, both non-surgical and surgical management strategies exist that attempt to reduce the buildup of extracellular lymph fluid within the affected limb and thus improve symptoms and reduce the risk of complications.
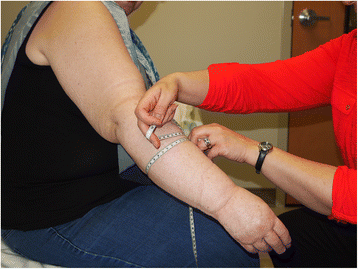
The main non-surgical management strategy, Complex Decongestive Therapy (CDT), includes manual lymphatic drainage, compression therapy, exercise and skin care as well as a range of motion, breathing and posture exercises, and education.
Surgical management strategies include ablative surgical methods, which aim at removal of the tissues affected by lymphedema, and physiological surgical methods, which aim to recreate normal or alternate avenues for lymph fluid to flow out of the affected limb.
Ablative surgical methods can be significantly invasive, and are directed towards the removal of the edematous superficial tissue layers of the affected limb. This includes the Charles procedure and suction-assisted lipectomy/liposuction. The Charles procedure represents a somewhat radical surgical procedure in which varying degrees of involved skin and subcutaneous tissue are excised from the affected limb, and can require coverage with skin grafts. Suction-assisted lipectomy/liposuction represents a much less invasive surgical procedure in which excess fat is removed from the affected limb using a suction cannula and liposuction device that is passed under the skin through multiple small incisions.
Physiological surgical methods are directed towards reducing the lymphatic fluid burden in the affected limb by either improving lymphatic circulation by introducing healthy tissue into the affected limb or creating an alternate outflow pathway for lymph fluid. These methods require using sophisticated microsurgical and super-microsurgical techniques, to accomplish the physical reconnection of lymphatic channels to either small veins in the affected limb, or healthy lymphatic channels or tissues that can be harvested from other parts of the body.
While currently available surgical management strategies can result in dramatic improvement in symptoms and quality of life for patients, many formidable challenges remain for successful management of secondary lymphedema. It is hopeful that ongoing clinical research efforts will ultimately lead to more complete and sustainable treatment strategies and perhaps a cure for secondary lymphedema, its debilitating symptoms, and its potentially devastating resultant complications.
What doctors in the Ohio and lower Mich are certified to do the surgical/lipsuction procedure? Mine is in my legs.
Only a limited number of surgeons across the United States perform these microsurgical procedures. Please feel free to contact the Plastic Surgery Department at The Ohio State University Wexner Medical Center in Columbus, Ohio for more information. Dr. Roman Skoracki is the Chief of the Division of Reconstructive Oncological Plastic Surgery, and he is a world leader in performing microvascular surgical procedures to treat the effects of lymphedema in cancer patients.